South Africa presents stark contrasts in public health. Breakthroughs like new obesity drugs coincide with affordability challenges. The 2026 agenda addresses obesity via GLP-1 medications, National Health Insurance (NHI) hurdles, AI innovations, tobacco controls, TB resistance, and HIV prevention strains.
Obesity Epidemic and GLP-1 Medications
About one-third of South Africans live with obesity, linked to non-communicable diseases (NCDs) including type 2 diabetes, hypertension, kidney disease, and certain cancers.
Last November, South Africa issued its first clinical practice guidelines for adult obesity treatment. These define obesity as a chronic disease and guide treatments from supportive care to medications and surgery.
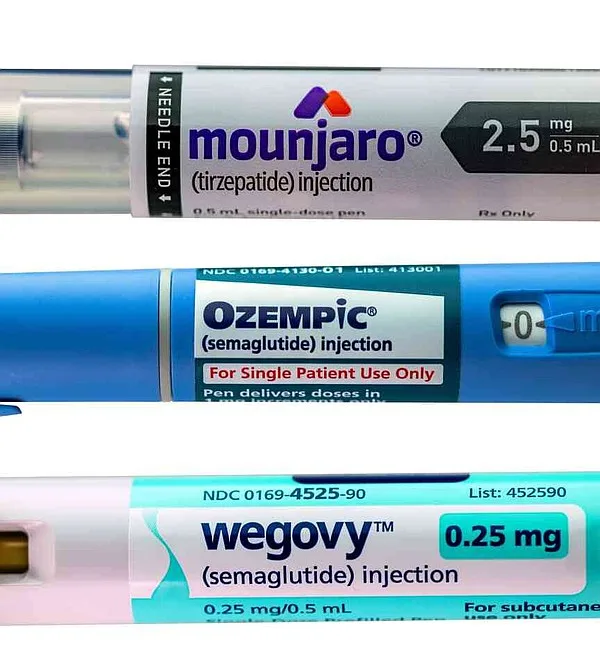
Guidelines recommend GLP-1 receptor agonists (GLP-1s), branded as Ozempic, Mounjaro, and Wegovy. These drugs lower blood sugar, slow digestion, and enhance satiety.
Approved for diabetes management in South Africa, Wegovy gained weight management approval last year. Experts view GLP-1s, used for diabetes over 20 years, as transformative for obesity.
Monthly costs range from R3,000 to R6,000, rendering them inaccessible for most. Unavailable in public health and not covered by medical aids for weight loss, patients pay out-of-pocket.
January research reviewing 37 studies found users regained all lost weight quickly after stopping after ~10 months. Like other chronic therapies, GLP-1 medications require lifelong use. Apps like Shotlee help track GLP-1 doses for consistent management.
Expert Insights on Obesity and GLP-1s
Angela Murphy, endocrinologist involved in guidelines:
The guidelines educate providers, doctors, nurses, government, and policymakers on obesity approaches. Up to 70% of obesity stems from genetics, not willpower. Lifestyle yields ~5% average weight loss; medications add key value.
Nomathemba Chandiwana, chief scientific officer, Desmond Tutu Health Foundation:
Obesity involves genetics, environment, and diet; treat it as a disease. GLP-1s need political will like HIV antiretrovirals. Drug makers like Eli Lilly (Mounjaro) and Novo Nordisk (Ozempic, Wegovy) must address pricing. Awareness campaigns educate on obesity, diabetes, and NCDs.
National Health Insurance (NHI) Stalls in Court
Signed into law in May 2024 after decades of debate, NHI aims to replace private schemes for 15% of South Africans and improve services for 85% reliant on public care.
Nine court challenges cite procedural flaws, funding issues, minister powers, and service failures. Constitutional Court reviews Ramaphosa's appeal; cases may consolidate and pause.
A Lancet Global Health Watch case study echoes concerns. Experts predict 2026 court delays, survival uncertain.
NHI Expert Views
Susan Cleary, health economist, University of Cape Town:
South Africa's current National Health Service model excels in funding. NHI brings change costs and flaws, granting excessive ministerial power without corruption safeguards.
Alex van den Heever, economist, University of the Witwatersrand:
NHI is unlawful as it promises unachievable outcomes. No analysis justifies restructuring; tax shifts ignore capacity limits.
AI Advances in Public Health
AI transforms diagnostics, data analysis, and research patterns. A Nature Genetics study showed AI predicting diseases years early.
AI aids TB screening via chest X-rays, tested in South Africa, enabling rapid hotspot detection.
Experts praise potential but caution on hype, stressing human oversight and data quality.
Precision tracking for your journey
Join thousands using Shotlee to accurately track GLP-1 medications and side effects.
📱 Get the Shotlee App
Track your GLP-1 medications, peptides, and health metrics on the go with our mobile app!
AI Perspectives
Thomas Hartung, Johns Hopkins professor:
AI computing doubles every three months. It processes millions of papers, accelerates drug development from 12 years/$3B to faster timelines. AI maps environmental health impacts via digital twins.
Siphamandla Gumede, researcher, Wits University:
AI enables networked health systems tracking clinic visits nationwide via alerts.
Guido Geerts, CEO Delft Imaging:
AI outperforms humans in TB X-ray reads after 30M cases but requires human checks for errors.
Tobacco Legislation Progress
The Tobacco Products Bill, started 2018, completed hearings August 2025. It bans displays, singles, public smoking, and regulates vapes similarly.
Industry resists plain packaging, warnings, and vape ads. Experts expect 2026 passage, possibly diluted.
- E-cigarette use rises parallel to smoking.
- Youth drawn to flavors/designs, not harm reduction claims.
- Illicit trade: Local firms underdeclare; track-and-trace needed.
Tobacco Experts
Lekan Ayo-Yusuf, University of Pretoria:
Industry pushes back on vape marketing bans despite evidence.
Corné van Walbeek, UCT professor:
60% tax evasion by locals; SARS track-and-trace can curb.
TB Challenges and Innovations
TB cases down 60% past decade, yet rates high. Over 50% carry latent TB; HIV, poverty fuel spread.
Rising bedaquiline resistance and funding cuts threaten gains. Advances: AI X-rays, targeted testing.
2018 survey: >50% TB asymptomatic, potential transmitters.
TB Research
Limakatso Lebina, Africa Health Research Institute:
Asymptomatic TB may drive transmission; research explores spectrum.
Mark Hatherill, UCT:
BCG wanes after 10 years. M72/AS01E (50% efficacy), MTBVAC candidates report 2028-2029; 30% effective better than none.
HIV Prevention Amid Funding Cuts
Lenacapvir (LEN), six-monthly prevention jab, rolls out alongside pharmacist ARV prescribing.
Key population services slashed; US funding cuts risk reversals after 20 years success.
HIV Expert Concerns
Simiso Sokhela, Wits University:
Drugs need delivery, education, fatigue management for marginalized groups.
Linda-Gail Bekker, Desmond Tutu HIV Centre:
LEN is not a vaccine; requires six-monthly injections like extended PrEP. Education prevents misconceptions.