When Weight-Loss Drugs Like Zepbound Don't Work
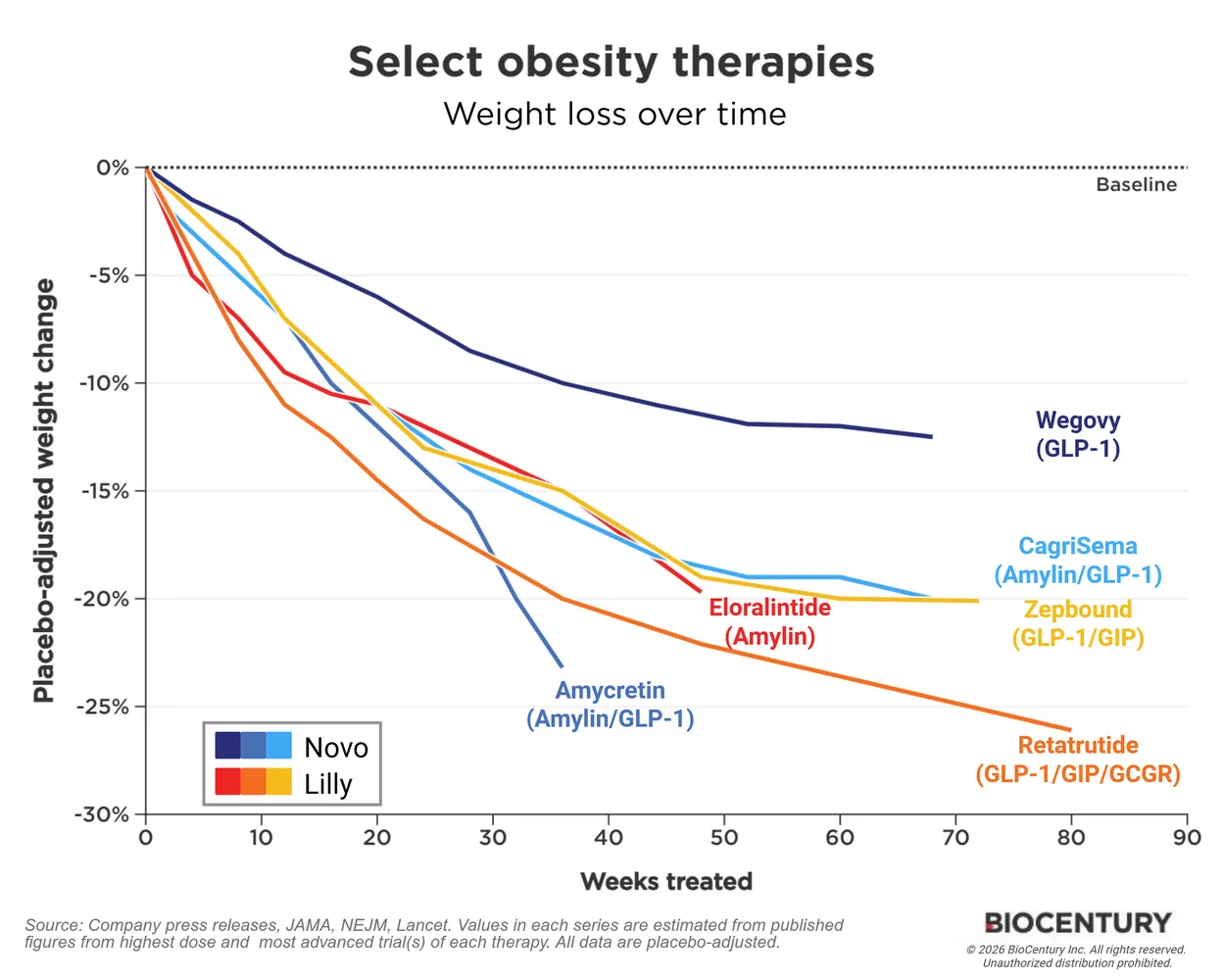
GLP-1 drugs like Zepbound and Wegovy have transformed weight management for millions, delivering average weight loss of 15 to 21 percent in clinical trials. Yet, for about one in 10 people—known as non-responders—these medications result in less than 5 percent body weight loss. When weight-loss drugs don't work, patients like Jessica Layeux face frustration after months of effort and expense.
The Real Story of a GLP-1 Non-Responder
Jessica Layeux, a 42-year-old cybersecurity expert from Monticello, Minn., started Zepbound last year hoping for significant results. Unlike many, she experienced no common side effects and noticed little change in hunger or cravings. Optimistic at first, she increased her dose but saw almost no weight loss over 15 months—only a pound or two.
Ms. Layeux began self-doubting, obsessing over injection sites, storage temperatures, diet, and exercise. At doctor visits, she eagerly shared her healthy habits to avoid blame. "No matter what I do, these 'miracle drugs' don't work," she said. "It felt extremely defeating."
Her experience highlights an overlooked reality: while GLP-1 agonists like tirzepatide (Zepbound) and semaglutide (found in Wegovy and Ozempic) help many shed significant weight, non-responders endure emotional and financial strain.
Understanding GLP-1 Drugs: How They Work and Why They Fail Some
GLP-1 medications mimic the glucagon-like peptide-1 hormone, which regulates appetite, slows gastric emptying, and promotes insulin release to control blood sugar. Semaglutide and tirzepatide primarily dial down appetite and silence "food noise" by targeting the brain's reward centers.
However, obesity stems from diverse causes beyond appetite. Clinical background shows these drugs excel for those with hyperphagia but less so for others. Non-responders may have obesity driven by metabolic, genetic, or inflammatory factors unrelated to food intake.
Genetics and Individual Response
Genetics plays a key role, influencing hunger, fullness, metabolism, and energy expenditure, said Marie Spreckley, a researcher at the University of Cambridge. Variations in genes related to appetite regulation, satiation, and metabolism can predict response.
Dr. Amy Sheer, an obesity medicine doctor at University of Florida Health, notes that people whose obesity isn't tied to overeating see diminished effects. Similarly, Megan Capozzi, a research assistant professor at the University of Washington Medicine studying diabetes and obesity, points to differences in eating pleasure affecting brain reward pathways.
Hormones and Biological Factors
GLP-1 drugs target only two hormones mainly involved in appetite and blood sugar, said Dr. Beverly Tchang, an obesity medicine doctor at Weill Cornell Medicine who consults for Novo Nordisk, maker of Wegovy. "When we think about the whole alphabet soup of hormones that control our weight, it's almost embarrassing to think that we can fix obesity by just addressing two."
Estrogen interacts with GLP-1 pathways, potentially heightening sensitivity—explaining why men may be more likely non-responders than women, and why hormone replacement therapy aids postmenopausal women, per Dr. Diana Thiara at University of California, San Francisco.
Precision tracking for your journey
Join thousands using Shotlee to accurately track GLP-1 medications and side effects.
📱 Get the Shotlee App
Track your GLP-1 medications, peptides, and health metrics on the go with our mobile app!
Timing and comorbidities matter too. Dr. Zoobia Chaudhry, director of the obesity medicine fellowship at Johns Hopkins Medicine, says longer obesity duration reduces efficacy. Type 2 diabetes patients struggle more, as do those with inflammatory conditions.
Predicting Non-Response: From Trials to Personalized Testing
Dr. Sheer waits four to six months before suggesting alternatives like bariatric surgery or medication switches. Recent trials analyzed genes for appetite, satiation, and metabolism, finding distinct profiles between GLP-1 responders and non-responders. Non-responders lost significantly on phentermine-topiramate, which acts differently on appetite-suppressing brain pathways.
Dr. Andres Acosta, obesity medicine physician at Mayo Clinic and senior author, advocates using patient traits to select first-line drugs. He co-founded Phenomix Sciences, offering a genetic test to guide choices. Though not proven in independent trials, some doctors use it post-GLP-1 failure.
Ms. Layeux's test revealed higher calorie needs for fullness and shorter satiety. Adding phentermine to Zepbound led to 20 pounds lost in a month.
What to Do If Weight-Loss Drugs Aren't Working for You
For patients, patience is key—give GLP-1s 4-6 months at optimal doses. Track progress meticulously; apps like Shotlee can log symptoms, side effects, injections, diet, and weight to share with providers.
Discuss genetics testing, dose adjustments, or combos like phentermine. Alternatives include other medications or surgery. Common side effects (nausea, GI issues) may resolve, but persistent non-response warrants reevaluation.
Compare options: Phentermine-topiramate suppresses appetite differently, suiting some non-responders. Always consult providers for personalized plans, weighing costs (thousands monthly for GLP-1s) against benefits.
The Future of Weight-Loss Treatments Beyond GLP-1s
New drugs targeting additional hormones are in development. Dr. Tchang reassures non-responders: "That doesn't mean we're not going to have it in six months, one year or two years."
Research into predictors promises tailored therapy, moving from trial-and-error to precision medicine.
Key Takeaways: What This Means for Patients
- 1 in 10 GLP-1 users are non-responders, losing <5% weight vs. 15-21% average.
- Genetics, hormones (e.g., estrogen), obesity duration, and diabetes influence response.
- Wait 4-6 months; consider genetic tests like Phenomix or switches to phentermine-topiramate.
- Track everything with your doctor—future multi-hormone drugs offer hope.
Conclusion
While GLP-1 drugs like Zepbound succeed for many, non-responders like Jessica Layeux underscore the need for individualized approaches. By understanding genetics, hormones, and predictors, patients can navigate setbacks toward effective solutions. Consult your obesity specialist to explore options and stay informed on emerging therapies.