Expanding Access to GLP-1 Weight-Loss Meds is Essential
Public health officials have long urged Americans to combat rising obesity rates through better eating, more movement, and healthier choices. Despite these efforts, obesity peaked at 40% of Americans in 2022. The subsequent decline is unmistakably tied to the emergence of GLP-1 medications, a breakthrough class of drugs transforming metabolic health.
The Obesity Crisis and Its Devastating Impact
Obesity drives a cascade of related conditions, including diabetes, heart disease, stroke, and cancer. These issues contribute to seven in 10 deaths annually in the U.S. and fuel a staggering $5.3 trillion in yearly healthcare costs. Traditional behavioral interventions have fallen short, unable to deliver sustained weight loss at scale.
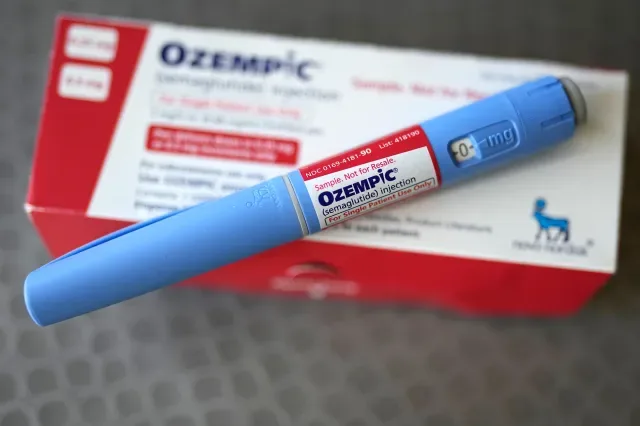
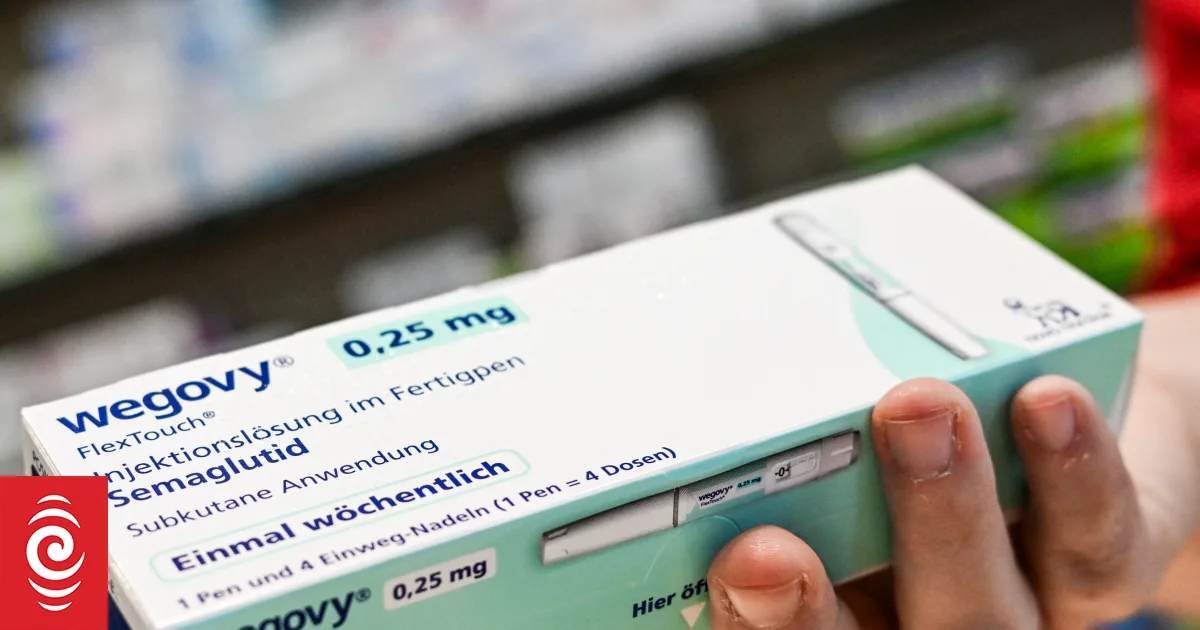
GLP-1 medications, such as semaglutide (found in Ozempic and Wegovy) and tirzepatide (in Mounjaro and Zepbound), change this equation. These drugs mimic the glucagon-like peptide-1 hormone, which regulates blood sugar, slows gastric emptying, and signals fullness to the brain. The result? Patients achieve 15% to 20% body weight loss—outcomes unmatched by diet and exercise alone.
How GLP-1 Medications Work for Weight Loss and Beyond
By activating GLP-1 receptors in the gut, pancreas, and brain, these therapies reduce appetite, improve insulin sensitivity, and promote fat loss while preserving muscle mass. Beyond weight reduction, they lower risks for type 2 diabetes, cardiovascular events, and even certain cancers. Clinical trials like STEP and SURMOUNT have validated these effects, showing sustained benefits with long-term use.
Groundbreaking USC Schaeffer Center Research on GLP-1 Access
Research from the University of Southern California's Schaeffer Center for Health Policy & Economics underscores the transformative potential of widespread GLP-1 access. For young adults starting treatment between ages 25-34, benefits include nearly two years of added life expectancy, nearly six fewer years with diabetes, and reduced risks of hypertension, heart disease, stroke, and cancer.
Even older adults benefit substantially. Medicare beneficiaries aged 65-74 starting GLP-1 therapy could gain about six months of life expectancy and spend less time managing diabetes complications.
Medicare Savings and Societal Benefits
Implementing Medicare coverage for GLP-1s would yield nearly $1 trillion in cumulative social benefits over the next decade. Medicare itself stands to save between $175 billion and $245 billion in the first 10 years, with 60% of savings stemming from fewer hospitalizations and reduced nursing home care. These projections account for drug costs offset by averted medical expenses.
- Life expectancy gains: Up to 2 years for young adults.
- Diabetes reduction: 6 fewer years for early starters.
- Cost savings: $175-245B for Medicare, $1T societal.
Addressing Health Disparities with GLP-1 Therapies
Obesity disproportionately burdens Black and Hispanic Americans, affecting 53% and 43% of each group, respectively. Limited access to GLP-1s exacerbates these inequities, as behavioral changes alone haven't closed the gap.
History offers a parallel: After beta blockers' approval in 1976, hypertension and cardiac disease rates dropped equally across income levels. GLP-1 medications can similarly bridge disparities in obesity management, making effective treatment available regardless of socioeconomic status.
Precision tracking for your journey
Join thousands using Shotlee to accurately track GLP-1 medications and side effects.
📱 Get the Shotlee App
Track your GLP-1 medications, peptides, and health metrics on the go with our mobile app!
Overcoming Barriers: Insurance Coverage and Costs
Currently, fewer than one-third of insurers cover GLP-1 medications for weight loss. Cash-paying patients can't apply those expenses toward insurance deductibles, creating a financial hurdle.
Critics cite high costs, but prices are plummeting. Injectable GLP-1s, once $1,300 monthly, have dropped 50% or more. A new once-daily GLP-1 pill starts at just $149 per month, potentially boosting adherence by simplifying dosing.
Safety Profile and Patient Considerations
GLP-1s are generally well-tolerated, with common side effects like nausea, vomiting, and diarrhea often improving over time. Rare risks include pancreatitis or thyroid tumors, prompting FDA monitoring. Patients should consult physicians to assess suitability, especially those with gastrointestinal issues or family history of thyroid cancer.
For optimal results, combine GLP-1 therapy with lifestyle support. Tools like Shotlee can help track symptoms, side effects, and medication schedules, empowering better management.
Who Should Consider GLP-1 Medications?
- Adults with BMI ≥30 (obesity) or ≥27 with comorbidities like diabetes or hypertension.
- Those failing behavioral weight loss attempts.
- Individuals at high cardiovascular risk.
Discuss with your doctor: Start low, titrate slowly, and monitor progress quarterly.
Comparisons: GLP-1s vs. Traditional Approaches
| Approach | Weight Loss | Sustainability | Health Benefits |
|---|---|---|---|
| Behavioral Interventions | 5-10% | Low at scale | Modest |
| GLP-1 Medications | 15-20% | High with adherence | Diabetes, CV risk reduction |
Unlike older drugs like phentermine, GLP-1s offer cardiometabolic protection, positioning them as a cornerstone of obesity care.
Key Takeaways: What This Means for Patients and Policymakers
- GLP-1s reverse obesity trends, delivering unmatched weight loss and longevity gains.
- Expanded access, especially via Medicare, promises massive savings and equity.
- Falling prices and oral options make coverage feasible now.
- View obesity as a biological disease, treatable like diabetes with insulin.
Conclusion: Time for Action on GLP-1 Access
Just as diabetes shifted from a 'lifestyle' label to a treatable condition with insulin, obesity demands the same recognition. Expanding insurance coverage for GLP-1 medications isn't just beneficial—it's essential for healthier lives, lower costs, and a more equitable society. Patients: Talk to your provider. Policymakers: Act on the evidence.
Alison Sexton Ward is a research scientist at the USC Schaeffer Center for Health Policy & Economics.