GLP-1s for Weight Loss: A Closer Look at Employer Coverage
The buzz around GLP-1 receptor agonists like semaglutide (Ozempic, Wegovy) and tirzepatide (Mounjaro) for weight loss is undeniable. These medications have shown significant promise in helping individuals manage their weight and improve metabolic health. However, a recent analysis by KFF sheds light on a growing concern among employers: the cost of covering these drugs.
Are employers rethinking their approach to covering GLP-1s? Let's dive into the key findings and explore what this means for you.
Employer Concerns and Coverage Adjustments
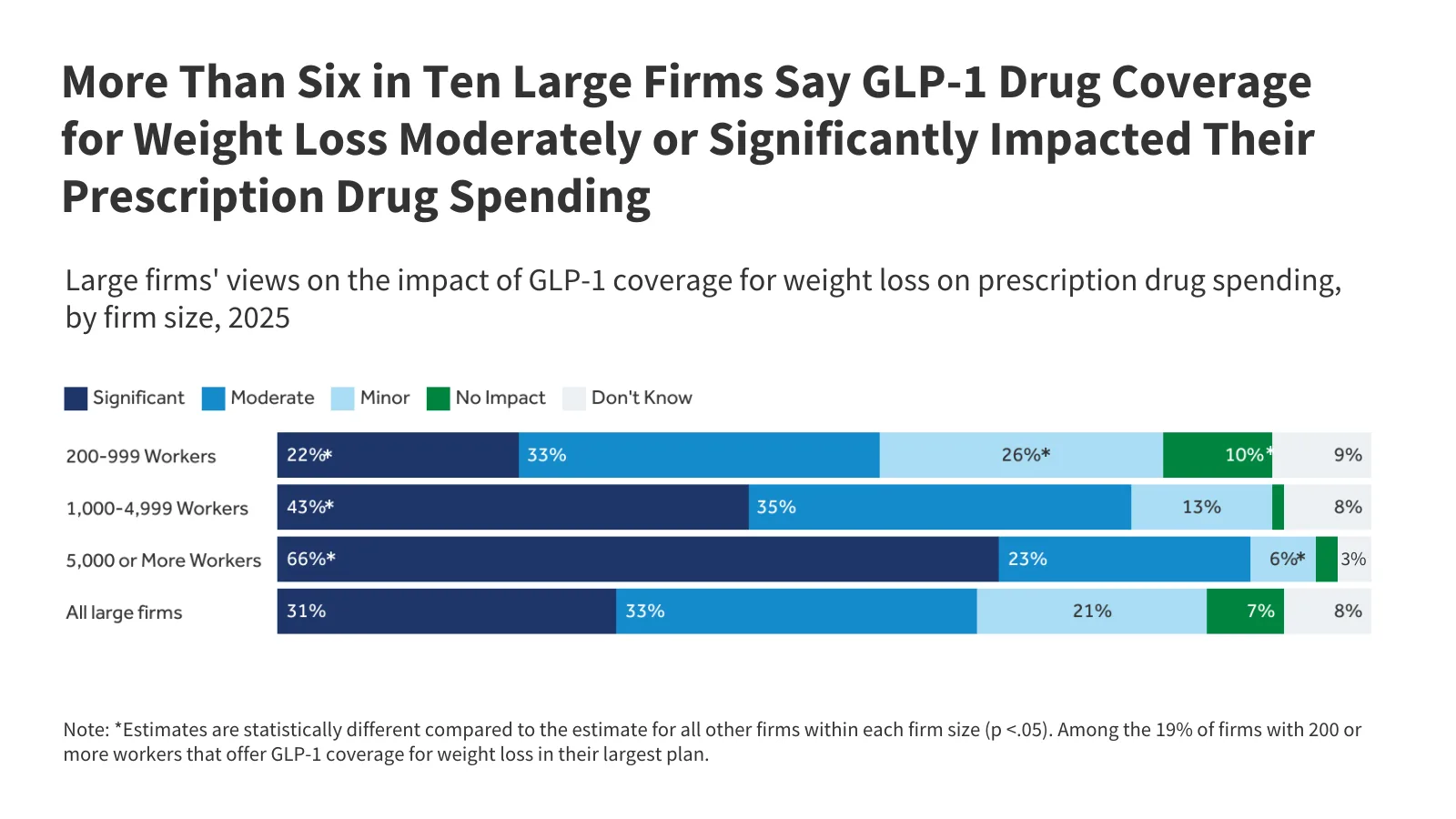
The KFF analysis, based on the 2025 Employer Health Benefits Survey and discussions with HR directors, highlights a prevailing unease about the financial implications of covering GLP-1s. Many employers are actively considering strategies to manage these costs, which could impact employee access to these medications.
Here's what employers are wrestling with:
- High Drug Costs: GLP-1s can be expensive, placing a significant strain on healthcare budgets.
- Coverage Requirements: To control costs, employers may be adding or strengthening coverage requirements, such as prior authorization or step therapy (trying other medications first).
- Potential for Scaling Back: Some employers are even considering reducing or eliminating coverage altogether.
The Broader Impact on Metabolic Health and Weight Management
The potential changes in employer coverage raise important questions about access to weight management solutions. While GLP-1s can be highly effective, they are just one piece of the puzzle. A comprehensive approach to metabolic health often includes lifestyle modifications like diet, exercise, and stress management.
Focusing on these core elements can have a positive impact and provide long term, sustainable weight management solutions.
Precision tracking for your journey
Join thousands using Shotlee to accurately track GLP-1 medications and side effects.
📱 Get the Shotlee App
Track your GLP-1 medications, peptides, and health metrics on the go with our mobile app!
Navigating the Evolving Landscape
So, what can you do to navigate these potential changes? Here are a few actionable takeaways:
- Understand Your Coverage: Check your employer's health plan details to understand the current coverage for GLP-1s and any requirements for access.
- Focus on Lifestyle Changes: Prioritize a healthy diet, regular exercise, and stress management techniques. These foundational elements can significantly improve your metabolic health, with or without medication.
- Talk to Your Doctor: Discuss your weight management goals and explore all available options, including lifestyle interventions and potential medication alternatives.
Could Peptide Therapy Be an Alternative?
Emerging research suggests potential benefits of other peptide therapies like BPC-157 for gut health and inflammation, which can indirectly support metabolic health. Exploring all available options with your doctor is vital.
Taking control of your health through education and a proactive approach is crucial, no matter the fluctuations in coverage.
The Role of Health Tracking
Tools like Shotlee can help track your progress and stay motivated. By monitoring your food intake, activity levels, and other key metrics, you can gain valuable insights into your health and make informed decisions.
Conclusion: Prioritizing Your Health Journey
The evolving landscape of GLP-1 coverage highlights the importance of taking a proactive and comprehensive approach to your health. By understanding your coverage, focusing on lifestyle modifications, and working closely with your doctor, you can navigate these changes and prioritize your long-term well-being. Remember, achieving optimal metabolic health is a journey, not a destination.