States Step In to Make Obamacare Plans More Affordable After Subsidy Expiration
In the wake of the federal tax credits for Obamacare plans expiring at the end of 2024, monthly premiums have spiked for millions, potentially doubling or tripling in cost. However, ten Democratic-leaning states—California, Colorado, Connecticut, Maryland, Massachusetts, New Jersey, New Mexico, New York, Vermont, and Washington—are using state funds to help residents afford coverage through their marketplaces. This assistance, some predating the federal cutoff, is saving enrollees hundreds of dollars monthly and stabilizing enrollment in key areas.
The Impact of Expired Federal Subsidies on Obamacare Enrollment
The enhanced federal subsidies, introduced via the American Rescue Plan Act in 2021 and extended through 2025 by the Inflation Reduction Act, were a temporary pandemic measure. They boosted Affordable Care Act (ACA) marketplace enrollment from 11.4 million in 2020 to 24.3 million last year, available to all regardless of income, with extra aid zeroing out premiums for some low-income households.
Congress allowed these subsidies to lapse on December 31, 2024. Federal data shows marketplace enrollment dropped by about 1.2 million by the end of last month compared to the prior year. The Congressional Budget Office projected 4.2 million more uninsured by 2034 without intervention.
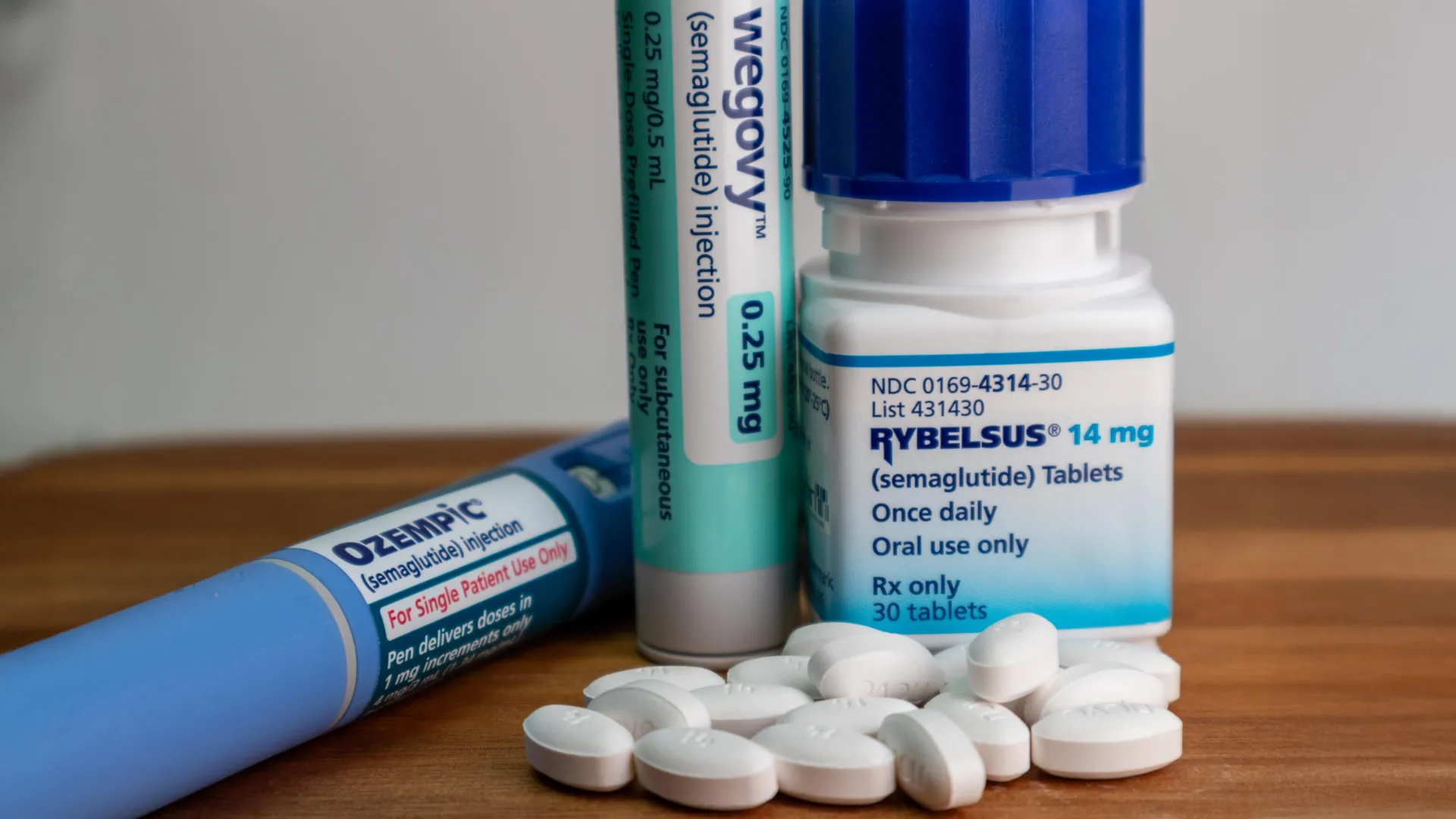
Compounding the issue are broader cost drivers, including labor shortages and soaring prescription drug prices. Notably, demand for GLP-1 drugs like Ozempic and Wegovy—used for diabetes and weight management—has driven up overall health care expenses, indirectly inflating Obamacare premiums as insurers adjust for pharmacy benefit costs.
Understanding GLP-1 Drugs' Role in Rising Premiums
GLP-1 receptor agonists such as semaglutide (Ozempic, Wegovy) mimic gut hormones to regulate blood sugar, slow gastric emptying, and promote satiety, aiding metabolic health. Their popularity for weight loss has exploded, with U.S. prescriptions surpassing 15 million monthly in recent peaks. This surge strains insurance formularies, as high list prices (often $1,000+ monthly before rebates) contribute to medical loss ratio pressures, leading to premium hikes across plans, including Obamacare marketplaces.
Patients on these therapies should discuss formulary coverage with providers, as state-based subsidies can help offset out-of-pocket jumps post-subsidy expiration.
State-Run Marketplaces: The Key to Local Subsidies
Under the ACA, states can use HealthCare.gov or run their own exchanges. Only the 21 states plus D.C. with state-run marketplaces can offer state-funded credits. At least ten are doing so to cushion the federal gap.
"Many of the people who buy Obamacare plans have fallen between the cracks of the health care system," said Matt McGough, policy analyst at KFF. "They might not work a job or work enough hours to be eligible for health benefits. They are too young for Medicare. They make too much for Medicaid, and they really have no other option but to go to the marketplace."
McGough warns that without aid, healthier individuals may drop coverage, leaving sicker enrollees and spiraling premiums—a "death spiral" states aim to prevent.
New Mexico: A Full Replacement Model
New Mexico stands out, fully replacing federal subsidies for all 82,400 marketplace enrollees through June 30 via its Health Care Affordability Fund. Gov. Michelle Lujan Grisham allocated an extra $17.3 million this year. Funded by a 3.75% surtax on insurers (expected to yield $165 million annually), the fund currently directs 55% to affordability, with plans to rise to 100% by 2028.