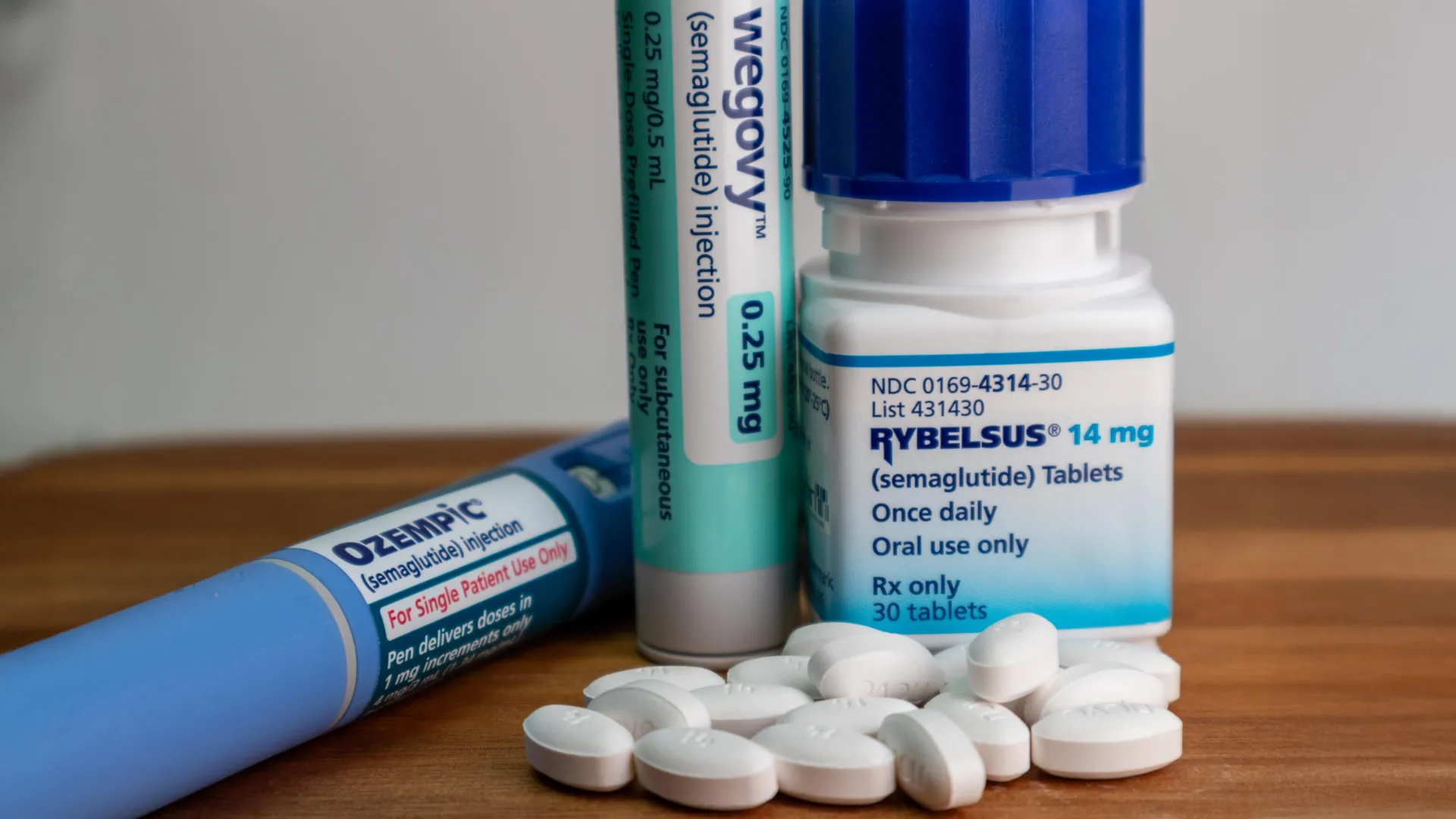
The Rising Popularity and Cost Burden of GLP-1 Drugs
GLP-1 drugs, such as Ozempic and Wegovy, have exploded in popularity for weight loss and metabolic health management. In the U.S., about 12 percent of adults say they're already on them. And worldwide, more than 25 percent of adults could benefit from the weight-loss treatment, according to new research from Mass General Brigham. These medications mimic the GLP-1 hormone to regulate blood sugar, suppress appetite, and promote significant weight loss—often 15-20% of body weight in clinical trials—making them highly valued for obesity and type 2 diabetes treatment.
However, their blockbuster status comes at a steep price, not just for users but for the broader healthcare system. Health insurers are passing along the cost for coverage in the form of higher rates across the board, warns Luca Maini, assistant professor of health care policy at Harvard Medical School. "If you look at the change in your health insurance premium this year over last year, about 30 percent of that is GLP-1s," Maini said in a recent Harvard Gazette interview.
Why Are GLP-1 Drugs So Expensive?
These drugs are expensive in part because they're effective, and patients value what they offer. But they're also patent-protected, so generic drug manufacturers can't produce these compounds for another few years. The companies that make these products are effectively monopolists.
Now, there is some competition, because there are a handful of these molecules that can be used for weight loss. And the price has come down quite a bit, even in the last few years. A recently approved Wegovy pill will cost $150 a month for patients without insurance. But we can expect the cost to remain relatively high, at least while the patents are in effect.
For context, GLP-1 agonists like semaglutide (the active ingredient in Ozempic and Wegovy) were initially developed for diabetes but gained fame for obesity due to their dual benefits on glycemic control and cardiovascular risk reduction. This efficacy drives demand, but limited competition keeps list prices high—often over $1,000 monthly before discounts.
Patient Guidance: Navigating GLP-1 Costs
If you're considering GLP-1 therapy, start by discussing eligibility with your doctor. Factors like BMI over 30 (or 27 with comorbidities), failed prior weight loss attempts, and metabolic risks determine suitability. Tools like Shotlee can help track medication schedules, symptoms, and side effects to optimize adherence and inform discussions with providers.
Variations in Coverage: Who Pays What for GLP-1s?
It depends on the type of coverage you have. Medicaid has very low out-of-pocket costs and covers virtually all drugs, but only a few states cover anti-obesity medications. Even patients in one of those states that do face substantial access restrictions. A Medicaid patient would need access to a physician who can write a prescription, and to go through administrative hurdles like prior authorization.
Medicare Part D, which is the part that covers prescription drugs, does not cover drugs that treat obesity—though that may be changing under the Trump administration's recent deals with manufacturers. The Trump administration in November announced new deals to lower the cost of the notoriously pricey drugs to a $50 monthly copay for people who rely on Medicare for health insurance.
Employer-sponsored plans tend to be more generous when it comes to coverage, but they also require more cost-sharing and, again, administrative hurdles like prior authorization. And lastly, out-of-pocket payers can access these drugs through the direct-to-consumer, telehealth services that are popping up online, which offer prescriptions at around $100 or $200 per month these days. The newly launched TrumpRX platform offers some GLP-1 discounts aimed at those who lack insurance or would pay more under their coverage.
Some states have ended coverage or restricted who qualifies for them under Medicaid plans due to these costs. For patients, this patchwork creates uncertainty—always verify your plan's formulary and prior authorization requirements.
The Disruptive Impact on Health Insurance Premiums
How disruptive have these drugs been for insurance companies? Well, it's certainly disruptive, but the solution, from the insurers' perspectives, is clear: Raise the cost of coverage, or at least the cost of insurance plans that cover these drugs.
One thing that's different about these drugs is that at least when it comes to treatment for obesity, patients can basically predict perfectly whether they'll need them, and that means the insurer can do the same thing. So it's actually fairly easy for them to figure out what kind of budget impact this will have on their bottom lines, and how much they need to raise premiums to make up the difference. That's already happening—about 30 percent of recent premium increases stem from GLP-1s.
Safety Considerations and Long-Term Use
GLP-1s are meant for long-term use, but evidence shows that as of now, GLP-1s have pretty unpleasant side effects, and a lot of patients stop taking them. Common issues include nausea, vomiting, diarrhea, and gastrointestinal discomfort, which can lead to discontinuation rates of 20-50% within a year. The financial impact may not be as steep as it would appear due to this adherence challenge. Patients should weigh these against benefits like improved cardiovascular health and monitor with their physician.
Comparisons to Other High-Impact Drugs
How unusual is it for so many patients to be eligible for a new class of drugs but face such a high cost? It's pretty much unprecedented, especially when you're talking about one in four adults being eligible for these drugs under the widest standards. The only comparison I can think of is statins [commonly prescribed to lower cholesterol]. A similar share of adults is eligible for those drugs, but much cheaper generics are available—and when they first came out, they weren't nearly as widely prescribed.
On the flip side, I'm reminded of the treatments for hepatitis C that arrived on the market a little more than 10 years ago. Of course, fewer people need treatment for hepatitis C, but the products were much more expensive when they first came out, so the burden on the healthcare system was comparable. What happened in that situation was that the drugs were heavily rationed—the natural solution, and the same thing is happening with GLP-1s. It's part of why the fully out-of-pocket, direct-to-consumer channel is so popular: because a lot of patients can't get the drug reimbursed through their insurance.
Uncertainties: Premium Trends and Broader Benefits
Should we expect those insurance premiums to keep going up or has the impact of GLP-1s mostly been factored in at this point? I would say the biggest adjustment has been factored in, though some uncertainty remains. The other factor is whether or not these drugs end up having benefits that reduce costs in other areas. Obesity is a comorbidity that tends to worsen other outcomes, whether that's cardiovascular health, risk of falls, things like that. So it remains to be seen how much money is saved if some of those outcomes are improved.
Global Perspectives on GLP-1 Access
How is this shaking out in other countries? The main difference is that in most other countries the fraction of people who would benefit from these drugs is smaller. Still, the majority of European countries, for example, have imposed very strict utilization controls, generally limiting use to patients with high body mass index.
Relief on the Horizon for GLP-1 Costs
Is there any relief on the horizon? Yes. In the short term, the Centers for Medicare and Medicaid Services, the federal agency that administers Medicare and partners with state governments to manage Medicaid, is testing what would happen if Medicare Part D covered GLP-1s for obesity—to get a sense for how much it would cost, and what those positive externalities might be.
And finally, even if it turns out these drugs have to be taken for life—and most people do—in about next five years or so, these patents will start to expire, and we'll have generic manufacturers making their own GLP-1s. At that point, they'll be very, very cheap. So even in the worst-case scenario, from a spending perspective, we can think of this moment as a very expensive blip.
Key Takeaways: What This Means for Patients and Policymakers
- GLP-1 drugs' high costs are contributing to 30% of recent U.S. health insurance premium increases, affecting everyone.
- Coverage varies widely: Medicare expansions and telehealth offer paths forward, but prior authorizations persist.
- Side effects drive discontinuation, potentially tempering long-term costs.
- Generics in 5 years promise affordability; compare to statins for perspective.
- Discuss with your doctor: Weigh benefits against costs and explore assistance programs like TrumpRX.
The GLP-1 revolution offers transformative potential for obesity and metabolic health, but its current price tag underscores the need for policy innovation. As patents expire and coverage evolves, patients can anticipate better access. Stay informed on your plan's updates, track your health metrics diligently, and advocate for sustainable solutions to ensure these drugs benefit society without bankrupting it.