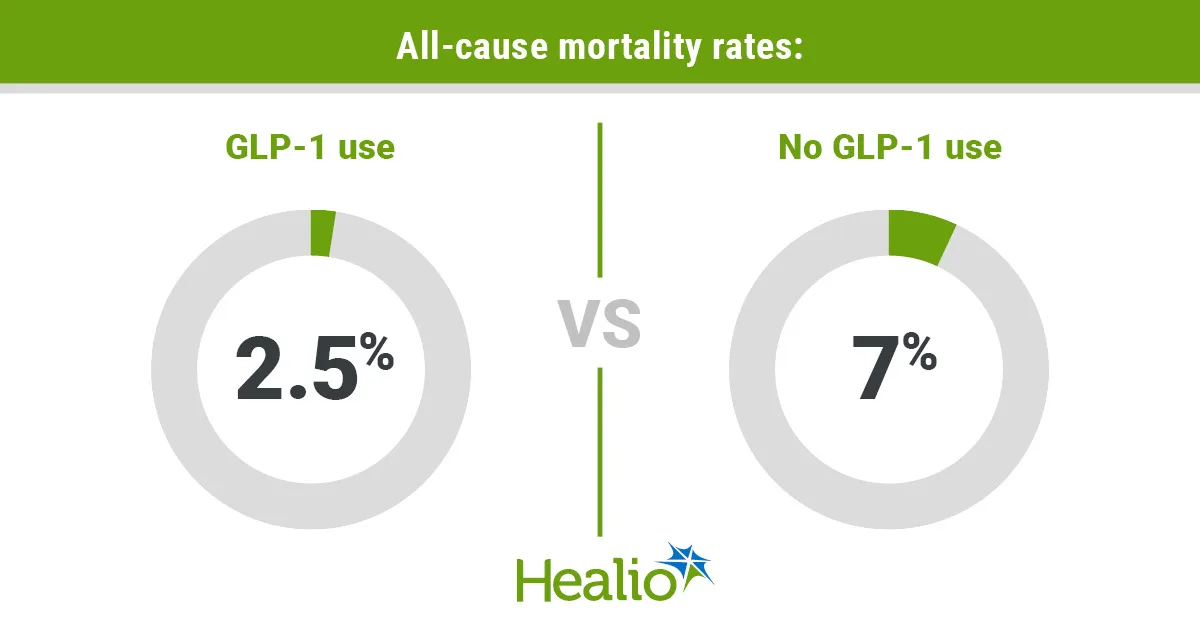
GLP-1 receptor agonists showed a strong link to reduced all-cause mortality in people with sickle cell disease, according to research presented at the ASH Annual Meeting and Exposition.
Patients using these medications also faced lower risks for sickle cell crisis, venous thromboembolism (VTE), ischemic stroke or transient ischemic attack (TIA), and cardiopulmonary complications.
Study Design and Cohorts
Asfand Yar Cheema, MD, resident physician at Cleveland Clinic Fairview Hospital, presented the retrospective analysis. "This study is retrospective, so we cannot conclude causality and there are many questions that need to be answered," Cheema told reporters. "However, it showed significant benefits, both in terms of individual patients' health but also from the perspective of the broader health care burden. These are intriguing, hypothesis-generating data."
GLP-1 receptor agonists have treated diabetes since 2005 and obesity since 2014. Prior research highlighted their anti-inflammatory, cardiometabolic, and endothelial-protective effects, including reduced inflammasome formation and oxidative stress—key factors in sickle cell complications.
"Sickle cell disease is fundamentally a vaso-occlusive and vasculopathic and thromboinflammatory disorder," Cheema explained. "We hypothesized that these overlapping mechanisms could benefit people with sickle cell disease."
Researchers analyzed TriNetX data from over 238,000 sickle cell patients treated between 2005 and 2022. Propensity-score matching created balanced cohorts:
Precision tracking for your journey
Join thousands using Shotlee to accurately track GLP-1 medications and side effects.
📱 Get the Shotlee App
Track your GLP-1 medications, peptides, and health metrics on the go with our mobile app!
- 4,807 GLP-1 users
- 4,807 non-users
Cohorts matched on age (median 53 vs. 55.9 years), sex (73.1% female both), race (76% Black/African American both), and comorbidities like hypertension (65.5% vs. 67.9%), diabetes (62.2% vs. 61.8%), and overweight/obesity (67.8% vs. 68.2%). HbA1c and other labs were also balanced. Follow-up lasted 3 years.
Key Outcomes
Primary outcomes showed significant reductions among GLP-1 users:
- All-cause mortality
- Sickle cell crisis
- Ischemic stroke/TIA
- Venous thromboembolism (VTE)
GLP-1 users also had lower risks for secondary outcomes, including:
- ICU admissions
- Hospitalization
- Acute kidney injury
- Thrombocytopenia
- Heart failure
- Pulmonary fibrosis
- Pulmonary hypertension
- Myocardial infarction
Limitations and Future Directions
The study noted limitations: retrospective design, ICD code reliance, and limited clinical granularity, preventing assessment of patient phenotypes or treatment histories. Causality remains unproven.
Still, findings are "compelling" and support prospective randomized trials to explore GLP-1s' disease-modifying potential in sickle cell disease therapy.
"GLP-1s are doing wonders in a variety of health care settings," Cheema said. "We know GLP-1 receptor agonists can possibly cause dehydration due to poor oral intake, and that promotes sickling, so the one area I was most intrigued by is the sickle cell crises. If you decrease them, heart failure exacerbation, pulmonary fibrosis and pulmonary hypertension will be reduced."