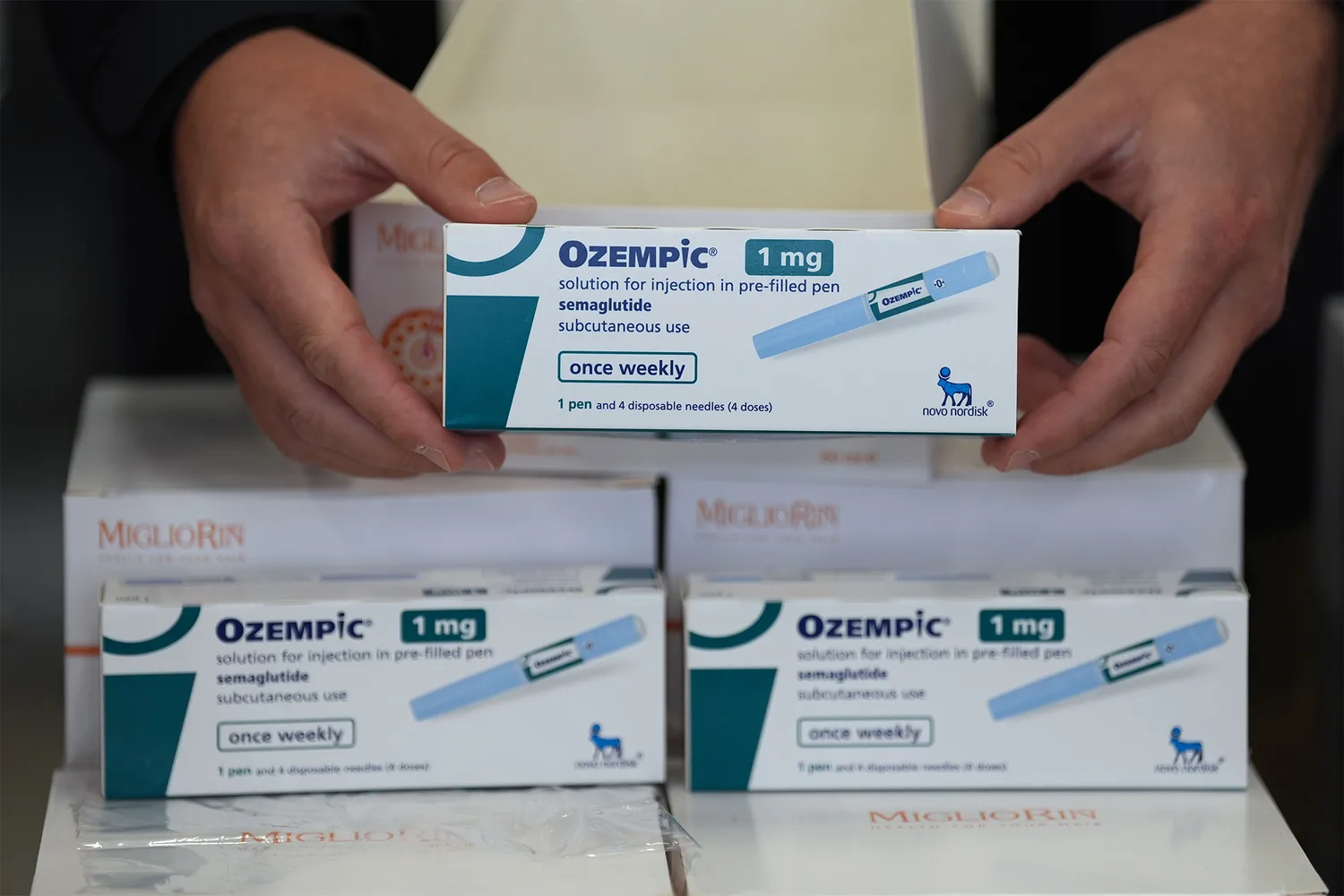
Impact on Californians
More than half a million residents in California might no longer have access to widely sought-after GLP-1 weight loss medications beginning January 1, 2026. This follows the state's decision to reject certain Medi-Cal reimbursements for these prescription treatments to reduce expenses.
Rise in Popularity of GLP-1 Drugs
GLP-1 medications have surged in demand among those seeking to shed pounds, especially since the Food and Drug Administration greenlit the branded drug Wegovy back in 2021. In 2023, California's Medi-Cal initiative, which supports low-income individuals and those with disabilities, funded treatment for more than 660,000 people using various GLP-1 drugs, as detailed by CalMatters.
Coverage Restrictions
The state will cease reimbursing for these medications when prescribed exclusively for weight reduction. However, coverage remains available for specific GLP-1 drugs if used to address other health issues, including diabetes, cardiovascular problems, or chronic kidney conditions. These adjustments affect branded options like Wegovy, Ozempic, Mounjaro, and Zepbound, based on a state announcement in November.
Uncertain Number of Affected Patients
It's unclear precisely how many Medi-Cal beneficiaries receive these drugs solely for weight management and will therefore forfeit coverage. The California Department of Health Care Services could not estimate this figure for the Los Angeles Times. A recent nationwide survey indicated that 38% of adults who have tried these treatments used them purely for weight loss, not to manage conditions like diabetes.
Precision tracking for your journey
Join thousands using Shotlee to accurately track GLP-1 medications and side effects.
📱 Get the Shotlee App
Track your GLP-1 medications, peptides, and health metrics on the go with our mobile app!
Broader Context of Budget Cuts
This reduction in coverage follows President Donald Trump's reduction of Medicaid funding by over $900 billion across the coming decade, limiting state resources for healthcare initiatives. Nationwide, states are implementing measures to economize within their Medicaid frameworks, such as limiting access to GLP-1 medications.
Proposed Savings and Additional Measures
Gov. Gavin Newsom's team suggested these reductions as a method to lower Medi-Cal expenditures. The state anticipates saving $85 million in the 2025-26 fiscal period and $790 million by 2028-29 through this GLP-1 adjustment. The governor's budget proposal also trimmed support in other domains, securing $1 billion by halting reimbursements for healthcare expenses of undocumented immigrants.
Recommendations and Concerns
Medi-Cal advises healthcare providers to gradually discontinue affected patients from GLP-1 drugs this autumn, then promote alternative approaches such as modifying diets, boosting physical activity, and seeking counseling. Health tracking apps like Shotlee can assist in monitoring progress with these lifestyle changes. Experts consulted by the LA Times warned that this policy shift could negatively affect Medi-Cal recipients, as many regain weight after ceasing GLP-1 use.